Why This Matters
For too long, women and girls experiencing severe menstrual pain have been told to “toughen up” or that it’s “just part of being a woman.” But for the estimated 1 in 10 women of reproductive age worldwide living with endometriosis, that pain isn’t normal — it’s a chronic, often disabling condition that affects health, relationships, work, and quality of life.
🧬 What Exactly Is Endometriosis?
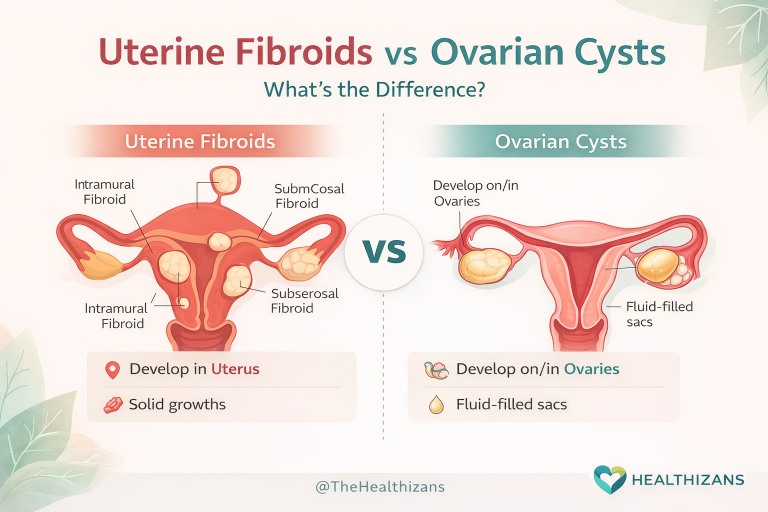
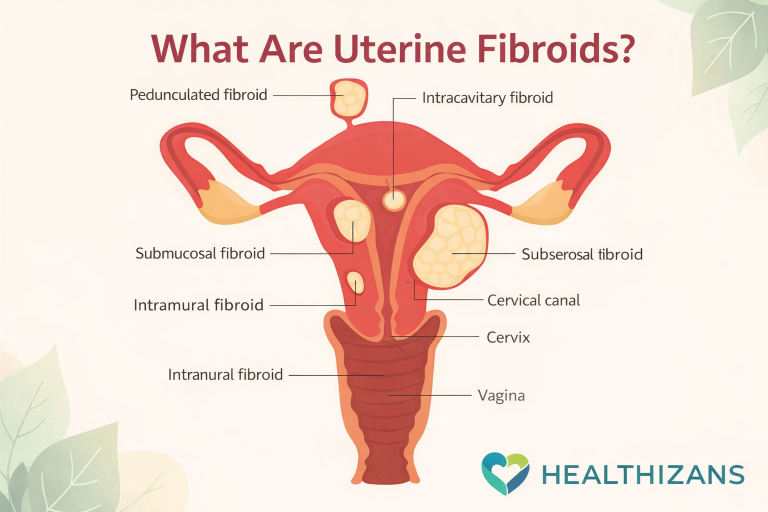
Endometriosis happens when tissue similar to the lining of the uterus (endometrium) grows outside the womb — often on the ovaries, fallopian tubes, pelvic lining, or even beyond.
This misplaced tissue behaves like the uterine lining: it thickens, breaks down, and bleeds with each cycle. But unlike menstrual blood that leaves the body, this blood has nowhere to go, causing:
- 🔥 Inflammation
- 🌱 Scar tissue and adhesions
- ⚡ Severe pelvic and back pain
🚨 More Than Just “Bad Periods”
Endometriosis symptoms vary, but common ones include:
- Debilitating period pain that interferes with daily life
- Pain during or after sex
- Chronic pelvic pain, sometimes outside menstruation
- Heavy or irregular bleeding
- Fatigue, bloating, and digestive issues
💔 Importantly, the average delay in diagnosis is 7–8 years in many countries (including the UK), as symptoms are normalised or misdiagnosed as IBS, stress, or simply “bad periods.”
🧠 The Hidden Impact on Mental Health
Living with relentless pain can take a toll on mental wellbeing. Research shows women with endometriosis have higher rates of:
- Anxiety and depression
- Social withdrawal
- Reduced work productivity (“endo costs the UK economy £8.2bn annually” – Endometriosis UK, 2020)
This highlights why endometriosis should be seen as a whole-body, whole-life condition, not just a reproductive disorder.
🩺 Diagnosis & Treatment Pathways
There’s currently no cure for endometriosis, but treatments can improve symptoms and quality of life.
- 🧪 Diagnosis: Often through laparoscopy (a minor surgical procedure), though MRI and ultrasound may support.
- 💊 Medical management: Hormonal therapies (like combined contraceptive pill, progestogens, or GnRH analogues) can reduce pain.
- 🔪 Surgery: To remove or reduce endometriotic tissue, improve fertility, or manage severe symptoms.
- 🌱 Lifestyle support: Anti-inflammatory diets, exercise, and stress management may help some women.
🌍 A Call for Awareness & Action
- WHO and NHS England both recognise endometriosis as a major women’s health priority.
- The UK Women’s Health Strategy (2022) specifically calls for improved research, faster diagnosis, and better support services.
The more openly we talk about endometriosis, the less likely women are to suffer in silence.
✅ Key Takeaways
- Severe period pain is not normal — it may be endometriosis.
- Average diagnosis delay is nearly a decade — awareness matters.
- Endometriosis affects fertility, mental health, and quality of life.
- Treatment is possible, even if there is no definitive cure.
❓ What’s Your Take?
Have you or someone you know struggled with getting answers for chronic pain or heavy periods? What changes would you like to see in how healthcare systems handle women’s pain? Share your thoughts — your voice matters.
📚 Sources
- WHO. (2021). Endometriosis Fact Sheet.
- NHS England. (2022). Women’s Health Strategy for England.
- Endometriosis UK. (2020). Endometriosis Costs Report.
- American College of Obstetricians and Gynecologists (ACOG). (2021). Endometriosis Clinical Guidance.