Scabies is a common but frequently misunderstood skin condition that affects millions of people worldwide each year. Despite how widespread it is, scabies is often surrounded by confusion, stigma, and delayed diagnosis — which can leave people dealing with relentless itching for weeks or even months.
The truth is simple: scabies is not caused by poor hygiene, and anyone can get it. Understanding what scabies is, how it spreads, and how it is properly treated is the key to stopping symptoms early and preventing reinfestation.
This guide explains scabies clearly, calmly, and without judgement.
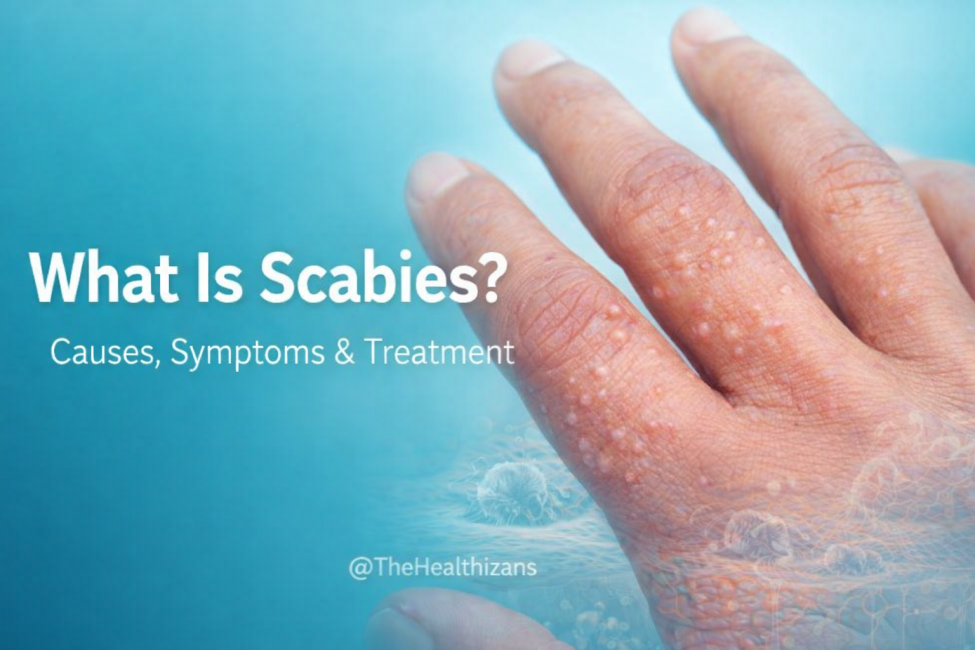
What Is Scabies?
Scabies is a contagious skin infestation caused by a microscopic mite known as Sarcoptes scabiei. These mites burrow into the outer layer of the skin, where they live, lay eggs, and trigger an immune reaction.
It is this immune response, rather than the mites themselves, that causes the intense itching and rash associated with scabies. Because the mites are invisible to the naked eye, scabies is often mistaken for eczema, allergic reactions, or fungal infections.
Scabies affects people of all ages and backgrounds and is particularly common in households, schools, care homes, and other settings where close contact is unavoidable.
How Does Scabies Spread?
Scabies spreads mainly through prolonged skin-to-skin contact. This includes living in the same household, caring for someone closely, or intimate contact. Brief or casual contact, such as a quick handshake, is far less likely to transmit the mites.
In some cases, scabies can spread through shared bedding, clothing, or towels — especially in crowded environments. However, scabies does not spread through food, water, or the air, and the mites cannot jump or fly.
Understanding this helps reduce unnecessary fear while focusing attention on what actually matters for prevention.
Symptoms of Scabies
Symptoms usually develop two to six weeks after the first exposure, although people who have had scabies before may notice symptoms much sooner.
The most recognisable symptom is intense itching, which often becomes significantly worse at night. This itching may be accompanied by small raised bumps, tiny blisters, or red patches. In some cases, faint burrow lines may be visible on the skin, though these are not always easy to see.
Scabies commonly affects areas such as the spaces between the fingers, the wrists, elbows, armpits, waistline, groin, buttocks, and feet. In adults, the head and neck are usually unaffected, although infants and older adults may show symptoms in these areas.
Repeated scratching can break the skin and increase the risk of secondary bacterial infections.
Why Is Scabies Itching Worse at Night?
Night-time itching is one of the hallmark features of scabies and often provides an important diagnostic clue.
This happens because the body’s immune response becomes more active during rest, skin temperature increases under bedding, and there are fewer distractions to take attention away from the discomfort. As a result, itching can feel overwhelming at night, leading to disturbed sleep and fatigue.
How Is Scabies Treated?
Scabies does not resolve on its own and requires proper treatment to eliminate the mites.
The most commonly recommended treatment is permethrin 5% cream, which is applied to the entire body as directed and usually repeated after seven days. In certain cases — such as widespread outbreaks or crusted scabies — oral medication like ivermectin may be prescribed.
One of the most important aspects of treatment is often overlooked: everyone who has had close contact with the affected person must be treated at the same time, even if they have no symptoms. Treating only one person allows the mites to circulate and is the main reason scabies appears to “come back”.
Managing Clothes, Bedding, and the Home
Once treatment has started, clothes, towels, and bedding used in the previous few days should be washed in hot water. Items that cannot be washed can be sealed in a bag for several days until any mites die off.
There is no need for deep cleaning, fumigation, or harsh chemicals in the home. Normal household cleaning is sufficient.
Recovery and What to Expect After Treatment
Itching may persist for two to four weeks after successful treatment. This does not necessarily mean the scabies is still present — it often reflects ongoing skin irritation and inflammation as the skin heals.
Moisturisers, soothing emollients, and avoiding scratching can help during this recovery phase. However, the appearance of new burrows, worsening rash, or spreading symptoms should be reviewed by a healthcare professional.
When to Seek Medical Advice
Medical review is important if symptoms do not improve despite correct treatment, if the skin becomes painful or infected, or if the affected person is pregnant, immunocompromised, or an infant.
Early treatment not only relieves symptoms but also helps protect others from infection.
Key Takeaway
Scabies is common, treatable, and nothing to be embarrassed about. Recognising the symptoms early, using the correct treatment, and treating all close contacts at the same time are the most effective ways to stop the itch and prevent reinfestation.
If a rash is persistent, intensely itchy, and worse at night, scabies should always be considered.
(You may also find our article on itchy skin conditions and rashes helpful )
What’s Your Take?
Have you or someone close to you ever dealt with a skin condition that was difficult to diagnose?
Sharing experiences can help others seek help sooner.
📚Sources
1. NHS – Scabies (Symptoms, Causes & Treatment)
2. World Health Organization (WHO) – Scabies Fact Sheet
3. Centers for Disease Control and Prevention (CDC) – Scabies Overview
4. British Association of Dermatologists – Scabies Patient Information Leaflet