Uterine fibroids are among the most common non-cancerous conditions affecting women of reproductive age, yet they are often misunderstood or dismissed as “just heavy periods.” In reality, fibroids can range from completely silent to life-disrupting, affecting menstrual health, fertility, comfort, and overall wellbeing.
This article explains what uterine fibroids are, why they develop, the symptoms that should not be ignored, and the treatment options available today, using evidence-based guidance aligned with organisations such as the NHS and the World Health Organization.
What Are Uterine Fibroids?
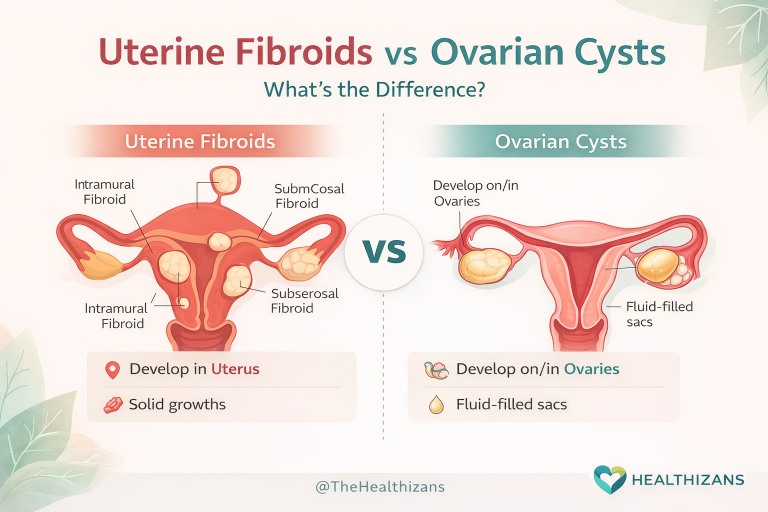
Uterine fibroids — medically known as leiomyomas or myomas — are benign growths made of muscle and fibrous tissue that develop in or around the uterus (womb).
They can vary widely in size and number. Some are so small they are never detected, while others grow large enough to alter the shape of the uterus or press on nearby organs. Importantly, fibroids are not cancer, and the chance of a fibroid becoming cancerous is extremely rare.
For many women, fibroids are discovered incidentally during a routine scan or pelvic examination. For others, symptoms are the first sign that something is not quite right.
Types of Uterine Fibroids
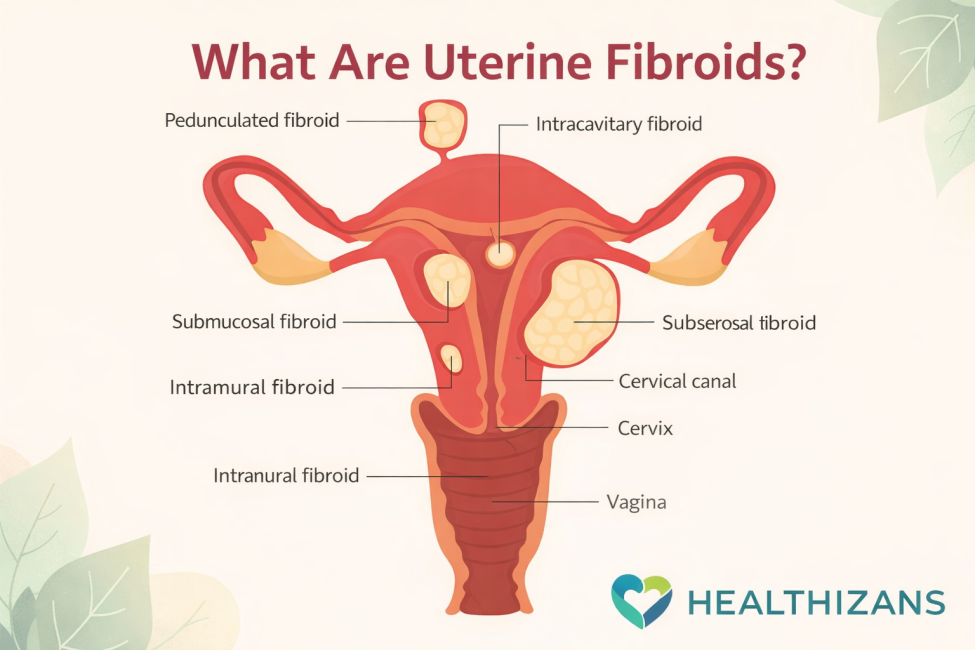
Fibroids are classified by where they grow, which often matters more than their size when it comes to symptoms.
- Intramural fibroids grow within the muscular wall of the uterus and are the most common type.
- Submucosal fibroids grow into the uterine cavity and are strongly linked to heavy or prolonged periods.
- Subserosal fibroids develop on the outer surface of the uterus and may cause pressure symptoms.
- Pedunculated fibroids are attached by a stalk, either inside or outside the uterus.
Understanding the type and location of a fibroid helps guide both symptom management and treatment decisions.
Symptoms: When Fibroids Become a Problem
Many women live with fibroids without any symptoms at all. However, when symptoms occur, they often develop gradually and may be mistaken for normal menstrual changes.
Common symptoms include:
- Heavy, prolonged, or painful periods
- Passing large blood clots during menstruation
- Pelvic pain, pressure, or a feeling of fullness
- Lower back pain
- Abdominal bloating or visible enlargement
- Frequent urination or difficulty emptying the bladder
- Pain during sex
Heavy bleeding is one of the most frequently reported symptoms. If your periods consistently disrupt work, sleep, or daily activities, it may be worth reading our article on heavy periods and when bleeding is no longer normal, which explains the warning signs that should not be ignored.
Over time, ongoing heavy bleeding may lead to iron-deficiency anaemia, a condition linked to fatigue, weakness, dizziness, and shortness of breath. We explore this further in our guide to iron deficiency anaemia, its causes, and early symptoms.
What Causes Uterine Fibroids?
There is no single cause of fibroids. Instead, research points to a combination of hormonal, genetic, and lifestyle factors.
Hormones play a central role. Oestrogen and progesterone appear to stimulate fibroid growth, which helps explain why fibroids are most common during reproductive years and often shrink after menopause.
Because of this hormonal link, fibroids may sometimes coexist with other hormone-related conditions. For example, women managing irregular cycles or hormonal imbalance may also experience overlapping symptoms — something we discuss in more detail in our article on PCOS, hormones, and menstrual health.
Other contributing factors include:
- Age (most diagnoses occur between 30 and 50)
- Family history of fibroids
- Early onset of menstruation
- Obesity
- Vitamin D deficiency
- Diets high in processed foods and red meat
These factors do not guarantee fibroids will develop, but they may increase susceptibility.
How Are Uterine Fibroids Diagnosed?
Fibroids are usually identified during investigations for symptoms such as heavy bleeding or pelvic pain, although some are found incidentally.
Common diagnostic tools include:
- Pelvic examination, which may detect an enlarged or irregular uterus
- Ultrasound, the first-line imaging test
- MRI scans, often used to map fibroids before treatment
- Hysteroscopy, which allows direct visualisation of fibroids inside the uterus
Accurate diagnosis helps determine whether fibroids should simply be monitored or actively treated.
Treatment Options for Uterine Fibroids
Treatment is highly individual. It depends on symptom severity, fibroid size and location, age, and whether future pregnancy is desired.
For women with mild or no symptoms, watchful waiting is often appropriate. Many fibroids remain stable for years without intervention.
Medications may be used to manage symptoms, particularly heavy bleeding or pain. These can improve quality of life but do not permanently remove fibroids.
Non-surgical procedures such as uterine artery embolisation (UAE) may be suitable for some women, as this reduces blood supply to fibroids and encourages shrinkage.
Surgical options include:
- Myomectomy, which removes fibroids while preserving the uterus
- Hysterectomy, which removes the uterus and is the only permanent cure for fibroids
Each option carries benefits and trade-offs, making shared decision-making with a healthcare professional essential.
Living Well With Uterine Fibroids
Having fibroids does not mean something is “wrong” with your body. Many women live full, active lives with them. What matters most is recognising when symptoms are no longer manageable and understanding that effective support is available.
If you are also planning a pregnancy or have concerns about fertility, fibroids may raise additional questions. You may find it helpful to explore our wider fertility-focused content, including articles on hormones, cycle health, and fertility planning, for broader context and reassurance.
What’s Your Take?
Have you ever been told that heavy periods are something you just have to “put up with”?
Or have fibroids ever been mentioned during a scan or routine check?
Sharing your experience may help someone else recognise the signs earlier.
🔗 Sources
- NHS Uterine fibroids (leiomyomas) – overview, symptoms, diagnosis, and treatment
- World Health Organization Women’s reproductive health and non-communicable gynaecological conditions
- Mayo Clinic Uterine fibroids: Symptoms and causes
- American College of Obstetricians and Gynecologists (ACOG)
Uterine fibroids – patient education and treatment options - Office on Women’s Health (U.S. Department of Health & Human Services)
Fibroids: causes, symptoms, and treatment