When it comes to women’s health, some conditions receive far less attention than they deserve. Vaginal cancer is one of them. Although it is rare, it can have serious consequences if symptoms are missed or dismissed — especially because early signs often resemble common issues such as infections or menopausal changes.
This article explains what vaginal cancer is, how it may present, what causes it, and how it is treated — in a clear, reassuring, and practical way.
Understanding Vaginal Cancer
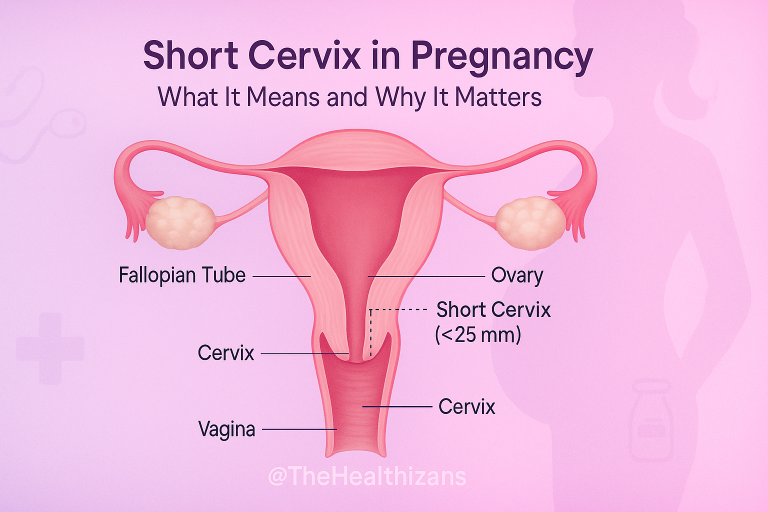
Vaginal cancer develops in the cells lining the vagina, the muscular canal connecting the cervix to the outside of the body. It is not the same as cervical or vulvar cancer, although these conditions affect nearby areas and may share similar risk factors.
Many women understandably confuse these conditions. If you’ve read our article on early signs of cervical issues, you’ll notice that while symptoms can overlap, the causes, diagnosis, and screening pathways are different — which is why accurate awareness matters.
Most vaginal cancers develop slowly over time, sometimes beginning as precancerous changes that go unnoticed for years.
Common types include:
- Squamous cell carcinoma – the most common type, usually affecting women over 60
- Adenocarcinoma – rarer and sometimes seen in younger women
- Melanoma and sarcoma – very rare forms
Because of its rarity, vaginal cancer is often not the first condition considered when symptoms appear.
Symptoms to Be Aware Of
Symptoms may be mild at first and easy to overlook. However, paying attention to changes in your body is crucial.
Possible symptoms include:
- Abnormal vaginal bleeding (particularly after menopause)
- Bleeding after sexual intercourse
- Unusual vaginal discharge (watery, bloody, or unpleasant-smelling)
- Pain during sex
- Persistent pelvic or vaginal pain
- A lump, sore, or mass in the vagina
⚠️ Key message: Any unexplained bleeding — especially after menopause — should always be checked by a healthcare professional.
What Causes Vaginal Cancer?
There is no single cause, but several factors can increase the risk.
Known risk factors include:
- Human papillomavirus (HPV) infection
- Increasing age
- Smoking
- A weakened immune system
- Previous cervical cancer or precancerous cervical changes
- Exposure to DES (diethylstilbestrol) before birth (mainly relevant to women born before the 1970s)
HPV is a major contributor, which is why vaccination and follow-up care play such an important role in prevention.
How Is Vaginal Cancer Diagnosed?
There is currently no routine screening programme specifically for vaginal cancer, unlike cervical cancer screening.
Diagnosis may involve:
- A pelvic examination
- Colposcopy (a closer examination using magnification)
- Biopsy to confirm cancerous cells
- Imaging tests (MRI, CT, or PET scans) to assess spread
This lack of routine screening is one reason symptom awareness and early presentation are so important.
Treatment Options Explained
Its treatment depends on several factors, including the cancer’s type, stage, size, and location, as well as the individual’s overall health.
Treatment options may include:
- Radiotherapy (the most commonly used treatment)
- Surgery to remove cancerous tissue
- Chemotherapy, sometimes combined with radiotherapy
- Supportive care to manage side effects and recovery
When detected early, treatment outcomes are often very good, even for this rare cancer.
Can Vaginal Cancer Be Prevented?
Not all cases can be prevented, but risk can be reduced.
Helpful preventive steps include:
- Receiving the HPV vaccination
- Attending regular gynaecological check-ups
- Avoiding smoking
- Practising safer sex
- Seeking medical advice promptly for unusual symptoms
Prevention is about being informed, not alarmed.
💬 Final Thoughts
Vaginal cancer may be uncommon, but women’s symptoms should never be minimised or ignored. Knowing what is normal for your body — and feeling confident to seek help when something changes — is one of the most powerful tools in women’s health.
❓ What’s Your Take?
Have you ever ignored a gynaecological symptom because you thought it was “probably nothing”? Your voice could help another woman feel confident enough to seek care.